; ?>/images/banner.jpg)

Sorry, no sugar coating here! Perhaps THE MOST IRRITATING part of my job as a veterinarian is when dog owners whose dog may not be particularly food motivated go out of their way find new foods to entice him to eat. Often, they resort for the most unhealthy dog food options that are loaded with fillers and sodium that may be attractive to the dog but in reality he would be better off being fed road kill. In other cases they resort to feeding people food and usually fail in providing well rounded nutrition.
Stop the madness people! Dogs will not starve. If they turn their nose up at food, leave it down for 30 minutes then pick it up and try again 12 hours later. If he refuses again, leave it down for 30 minutes and again pick it up…and so on. I guarantee you they within a day or two he will figure out that this is all he is getting fed, this when he is getting fed, and he has a finite period of time to eat it. In this manner YOU will dictate when and what the dog eats, not the other way around.
During the times a dog refuses food, with few exceptions, it will not harm their health. The one exception is toy breed puppies up to about 3 months of age that can be prone to hypoglycemia (low blood sugar). Other than than that, all that may happen is that the dog may lose a little weight which is probably a good thing, because more often than not, these dogs that have their appetite catered to ironically are overweight and even morbidly obese.
My favorite is when a recommend a weight control diet for a dog that is morbidly obese and was fed everything under the sun and the owner calls stating that the dog dog won’t eat the diet. My answer is always, GOOD! Great way to start a weight loss program!
Dr. Roger Welton is a practicing veterinarian and highly regarded media personality through a number of topics and platforms. He is the author of The Man In The White Coat: A Veterinarian’s Tail Of Love. In addition to being passionate about integrative veterinary medicine for which he is a globally recognized expert, Dr. Welton was also an accomplished college lacrosse player and remains to this day very involved in the sport. He is president of Maybeck Animal Hospital , general partner of Grant Animal Clinic, and runs the successful veterinary/animal health blogs Web-DVM and Dr. Roger’s Holistic Veterinary Care. Dr. Welton fulfills his passion for lacrosse through his lacrosse and sport blog, The Creator’s Game.

While many small businesses are experiencing major slow downs in business during the coronavirus pandemic, the trend in veterinary clinics across the nation is opposite. Across the country, my clinics included, are experiencing record caseloads with many veterinary clinics booked out days to weeks in advance and operating well beyond capacity. It is not unusual to hear about 24 hour emergency veterinary hospitals to have wait times exceeding 4 plus hours. What it is about the COVID-19 era that is causing so many pets requiring veterinary clinic visits?
Pet Owners Noticing More
Dogs and cats by their nature hide signs of illness and pain. Thus in the flow of many pet owners’ busy lives, subtle signs that something may be wrong with the health of family pets commonly go unnoticed. It often takes more obvious signs like limping in pain, diarrhea, vomiting, and prolonged anorexia to prompt busy pet owners to schedule a veterinary visit.
With many states having had shelter in place rules and many people still working from home, people are simply paying more attention to their pets and picking up on subtle signs of disease such as drinking more water than usual, eating less, eating more, urinating more frequently, mild limping, etc. Often, even subtle signs such as these are the consequent of series underlying disease and owners picking up on them have enabled more frequent early disease detection.
Spike In Pet Fostering, Adoptions
The coronavirus pandemic had nudged many to take the plunge to adopt a new pet they’d been thinking about getting given the unusual opportunity to be at home to acclimate the pet. Out of shear boredom and wishing to use their time productively, many animal enthusiasts found a unique COVID-19 induced capacity to take on rescue fosters. Whether adopted or fostered, these pets require care and represent a significant proportion of new pet veterinary clinic visits.
COVID-19 Forced Clinic Shutdowns
Veterinary clinics with COVID-19 positive staff members sometimes are required to shutdown causing a spike in requested veterinary visits at neighboring clinics. Within a 5 mile radius of the busiest of my two clinics, 3 large veterinary clinics have been forced to closed for weeks at various times over the past few months. Each time this has occurred we have experienced dramatic spike in case loads.
Please Be Patient!
Most of us are doing our very best to accommodate sick and injured patients. Between the surge in visits and having to operate with curbside service with only staff and patients allowed in the building, there are inevitable delays. We ask for your patience and understanding as we do everything in our power to serve you and your pets.
Please also show some empathy to the technicians and doctors running in and out of the building sweating in their PPE, logging more steps than most peoples’ epic workouts. Also, please do not complain that you cannot come in with your pet! We are doing what we are required to do by our respective state veterinary medical associations to remain open!
Dr. Roger Welton is a practicing veterinarian and highly regarded media personality through a number of topics and platforms. He is the author of The Man In The White Coat: A Veterinarian’s Tail Of Love. In addition to being passionate about integrative veterinary medicine for which he is a globally recognized expert, Dr. Welton was also an accomplished college lacrosse player and remains to this day very involved in the sport. He is president of Maybeck Animal Hospital , general partner of Grant Animal Clinic, and runs the successful veterinary/animal health blogs Web-DVM and Dr. Roger’s Holistic Veterinary Care. Dr. Welton fulfills his passion for lacrosse through his lacrosse and sport blog, The Creator’s Game.
 As medical marijuana becomes legal and accessible to more people in more states, pet owners are looking for ways they can use this new family of medications to help their pets. In humans, marijuana and hemp products, and their extracts, are being touted to treat a wide variety of syndromes and diseases. I know individuals who suffered from seizures, or chronic pain, and their lives have dramatically changed for the better, thanks to cannabis-made medications. Fortunately, there are well-designed studies to back up many of these claims…in people.
As medical marijuana becomes legal and accessible to more people in more states, pet owners are looking for ways they can use this new family of medications to help their pets. In humans, marijuana and hemp products, and their extracts, are being touted to treat a wide variety of syndromes and diseases. I know individuals who suffered from seizures, or chronic pain, and their lives have dramatically changed for the better, thanks to cannabis-made medications. Fortunately, there are well-designed studies to back up many of these claims…in people.
When it comes to pets, we aren’t so lucky. Can we extrapolate human data to apply it to dogs and cats? We do with many other drugs quite often, but we must be cautious. Does the law allow for pets to use medical marijuana? The laws are rather silent on pets, making it more risky. Here’s a breakdown.
A quick internet search for legitimate information on cannabis products for pets yields primarily companies selling these products. Obviously, they will tell you their particular product or brand is superior to the others, and their product will treat, manage, or even cure a long list of diseases. We need to wade through the advertising and self-promotion and get down to facts.
CBD, THC, cannabinoids…the basics
Marijuana and hemp are plants in the genus Cannabis. Many different species and strains of these plants exist, and almost 500 different compounds have been isolated from these plants, all with potential medicinal uses. Of these, over 80 are classified as cannabinoids. Different plants contain varying levels of cannabinoids and other compounds.
Every chemical has its own unique properties, and much more research will be needed for us to understand the full potential of this array of potential medications. For our purposes, there are two main cannabinoids that you’ll see mentioned the most: CBD and THC. CBD (cannabidiol) is the “medicine-y” cannabinoid. It’s extracted from a hemp plant, but lacks the psycho-active effects most people think of when they think of marijuana. The molecule responsible for that “high” one can get from marijuana is the other cannabinoid called THC (TetraHydroCannabinol). Think of CBD as the president of the science club, and THC as the party girl, if that helps.
The marijuana plant contains more THC, the chemical responsible for the “high”, while the hemp plant is more fibrous, and contains very little THC. Instead, hemp’s main compound is CBD. What makes us call one plant hemp and the other marijuana if they are both in the same family? Basically, more THC earns it the name “marijuana” while less THC (<0.3% depending on who you read) makes the plant hemp, or even “industrial hemp.”
There are also synthetic cannabinoids out there. The laws are more lax on these, making them “less illegal”, as most of the rules the DEA makes are about the compounds extracted from Cannabis plants (see below). Two of them are actually FDA approved (for human use!) Marinol is prescribed to help AIDS patients not lose their appetites and maintain body weight. Cesamet is prescribed to patients undergoing chemotherapy to help reduce the nausea and vomiting which can happen too commonly. It’s also being used (again, in people) to treat chronic pain and even Irritable Bowel Disease!
While these synthetic cannabinoids sound like a great thing, patients taking them report they don’t seem as effective. Apparently, the synthetics contain one and only one compound, while the extracts contain mainly that compound, but have other cannabinoids along for the ride that seem to have an additive effect. So, bottom line, the products from plants, as of now, seem to work better.
Giving cannabinoids to pets
I know very few veterinarians who recommend these products, for a variety of reasons. Little to no data exists on what dose is safe and/or effective. Little is known about drug interactions. Next to nothing is known about long-term use, simply because the state laws allowing us to conduct large scale clinical trials with it are relatively new. There is absolutely no regulation of production of these products, so we have no way of knowing if what is claimed on the bottle is what actually is in the bottle. Finally, the constant changing of the legal status of these products makes many veterinarians want to keep their noses clean and avoid the whole legal mess until the federal and state laws can come to some agreement.
Here’s a taste of what we do know.
CBD has great promise in the treatment of seizures, but appears to be poorly absorbed into dogs’ bodies when given orally. As far back as 1988, we knew cannabinoids had great potential as a treatment for seizures. Six dogs were given the CBD through an IV, then orally to compare. The IV doses were absorbed into the blood stream and eliminated via the liver. The medication hung around a while too, with a half-life of 9 hours! The oral dosing was not at all absorbed (none detected in the bloodstream) in half the dogs, and the other three that did absorb it had negligible levels. This study was only of six dogs, so we cannot draw any major conclusions from it. Yet, it does not seem promising for CBD’s as an oral option, unless presented in a different version or compound than the one used. Obviously, much more research needs to be done. (Pharmacokinetics of cannabidiol in dogs. Drug Metab Dispos. 1988 May-Jun;16(3):469-72.)
CBD might inhibit the cytochrome P450 enzyme. Here’s the research on it. Not a bad paper, but everything was done in vitro, (where most research starts) and nothing performed in an animal. Chemicals can behave differently than cells in a liver. And what is cytochrome P450 and why do we care? Oh, you care! This is a very important enzyme in the liver that is responsible for metabolizing (breaking down) medications or toxins. If this enzyme is inhibited and your pet is on other medications, it could, theoretically, cause the circulating dose of those other medications to increase, which is not always a good thing.
Dogs may have up to ten times more CB receptors than humans. In order for any chemical to interact with a living organism, there have to be receptors on the cells somewhere in the body. Imagine a catcher’s mitt that has a unique shape that only a certain size and shape of ball can fit into. That is what the cells in our brains, liver, and even skin have. For example, glucose receptors seek out glucose and bind to it. The CB receptors are like catchers mitts sitting on the cells and waiting for a cannabinoid molecule to be caught. When it is, the cell absorbs the molecule, chemical reactions happen, all kinds of magic. Bottom line – the more receptors an animal, or even an organ, has, the more sensitive that animal, or organ, is to that chemical. With dogs having 10 time more receptors for cannabinoids than people, they could potentially be 10 times more sensitive! This must be taken into account for both dosing, and thinking of side effects. (Houghston, SW Vet Symposium 2016)
So, take the first paper into account, where the CBD’s did not seem to enter the bloodstream of dogs when given orally. Now we know dogs have 10 times more CB receptors than people. How the heck do we decide on a dose?
That is precisely the problem.
CBD has been shown to reduce seizures in rats. We’ve also learned, anecdotally, that cannabinoids help epileptic humans as well. We suspect it works by inhibiting the CB receptor, and/or reducing calcium fluxes in neurons. (Izzo AA. Non-psychotropic Plant Cannabinoids: New Therapeutic Opportunities from an Ancient Herb. Cell Press, Elsevier; 2009:515–527.)
CBD may be a potent neuroprotector. Once nerve cells die, they are gone forever. This is why brain damage of any kind, in any species, is such a big bad deal. Izzo et al suggests CBD’s may prevent brain cell death in certain situations, and can even reverse brain damage resulting from lack of oxygen… in rats.
Lesser-known cannabinoids (CBC and CBG) have demonstrated great antimicrobial activity. With all the antibiotic resistant bacteria we have in the world, a new medication that can possibly kill “super-bugs” would be wonderful!
There are many other great studies out there on rodents, giving us hope for future applications. However, it’s a start, and much more needs to be done.
So what is legal, and what isn’t?
And why is this so complicated?
Web-DVM guest blogger Dr. Karen Louis is a practicing small animal veterinarian. See more of her articles at her blog at VetChick.com
 Death and loss of life is a regular part of being a veterinarian, yet it never ceases to hurt when we lose patients. However, no one lives forever and inevitably we are faced with disease circumstances for which there is no cure.
Death and loss of life is a regular part of being a veterinarian, yet it never ceases to hurt when we lose patients. However, no one lives forever and inevitably we are faced with disease circumstances for which there is no cure.
It hurts even more when we deduce from the diagnostic evidence at hand that there is reason to be hopeful but the case plays out nonetheless in a far less hopeful direction. Beyond that, it is more difficult when it is a cherished patient I have had the pleasure of knowing for most of his life, owned by a cherished client.
In 2006, a beautiful, helpless black kitten was found in a dumpster by one of my technicians. We were all taken by his remarkable affection despite having likely known nothing but hardship in his first 8 weeks of life. As we nursed him back to health, the techs affectionately named him McLuvin (from the movie Superbad that was popular at the time).
In a short period of time, word about McLuvin reached a dear client who adopted him, later to change his name to Captain Jack. Throughout his life, Captain Jack remained the lover he was as a kitten and it was always my pleasure to see him for over a decade for his well visits. Last week, Captain Jack came in for unexplained weight loss. Physical examination revealed a mid-abdominal, large, freely movable mass. Between how it felt and its location on a follow up x-ray, it appeared the mass emanated from his spleen.
The most common cancer of the spleen in cats is lymphoma, a systemic cancer that is very treatable in an inexpensive and minimally invasive manner following surgical resection of the spleen and attaining a diagnosis. That was the plan going in.
Upon surgically exploring the abdomen, I quickly realized that the large mass was not from the spleen at all, but was a pendulous mass that was projecting from one of his liver lobes. I proceeded to remove the mass via liver lobectomy and closed and recovered my patient without incident.
Everything seemed fine until the next morning when Captain Jack became hypothermic and poorly responsive for reasons we could not quite figure out. But after warming him and administering fluids, Captain Jack rallied, started eating, was purring and playful within a day and went home. I was excited for the biopsy report to come back Monday to see what further measures I could enact to further along his quality of life and longevity.
I returned Monday with the notification that Captain Jack passed away at home over the weekend. It was crushing for me to hear and I called the owner who I hold in very high regard to offer my condolences and give her the biopsy report if she still wanted to know what the nature of the mass was. I reported that it was a cholecellular carcinoma, a rare and aggressive cancer for which further treatment would not have been able to realistically stop or even slow significantly. Captain Jack never really had a chance at all.
The owner took the news well and she must have noted the sad tone of my voice when she said, “Please don’t feel bad, you did everything you could. You fought for him and I thank you for that.” From her perspective as a human nurse, she added, “Sometimes things just get beyond our control.”
Usually playing the role of consoler, this may have been the first time I had an owner console me over the loss of her pet. I really appreciated that and it set the tone for me to shake it off, go about my day, and fight for more pets to the best of my ability.
Dr. Roger Welton is a practicing veterinarian and well regarded media personality through a number of subjects and platforms. In addition to being passionate about integrative veterinary medicine for which he is a nationally renowned expert, Dr. Welton was also an accomplished college lacrosse player and remains to this day very involved in the sport. He is president of Maybeck Animal Hospital , runs the successful veterinary/animal health blogs Web-DVM and Dr. Roger’s Holistic Veterinary Care, and fulfills his passion for lacrosse through his lacrosse and sport blog, The Creator’s Game.
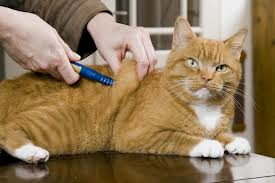 I can’t think of a disease that causes more owner anxiety than diabetes. Something about having to give a shot twice a day, every day, to an animal you love is very daunting. Then you do it a couple times and suddenly, it’s a breeze! I’ll try to help you get “breezy” fast!
I can’t think of a disease that causes more owner anxiety than diabetes. Something about having to give a shot twice a day, every day, to an animal you love is very daunting. Then you do it a couple times and suddenly, it’s a breeze! I’ll try to help you get “breezy” fast!
Insulin is kept in the refrigerator. Some pens made for humans can be left out for periods of time, but for the most part, plan on refrigerating the insulin. If you have a decent drive to the pharmacy or vet office, bring a little cooler to bring the insulin home. It needs to be gently mixed before each dose. Vetsulin, an insulin made specifically for dogs and cats, can be shaken like a polaroid picture. Other insulins need to be gently inverted in a rocking motion, not shaken like orange juice.
Your veterinarian will show you how to give shots, and make sure you get some practice with saline solution! Here’s some pointers (hoping to have a video soon!):
If multiple people will be giving the shots, I suggest having a pow wow on measuring the insulin. 3 units to my eyes might look like 3.5 to yours. So, get everyone on the same page.
Pick a time (two times actually, 12 hours apart) and stick with it. Most people do 7 am/7pm or something similar. I have a client who works late and gives the insulin at midnight and noon! Do what works with your schedule. I often feed the animal first, make sure they eat, then give the insulin. Some veterinarians recommend giving the shot 30 minutes before a meal. That makes the most sense biologically, but then what if the pet doesn’t eat? You have insulin in them that you can’t get out! And now we worry about their blood sugar dropping too low. If we make sure they eat before giving the shot, that’s a non-issue.
Here’s how to handle other common questions:
How can you tell if it’s working? How do you know when to worry? coming up are my articles on monitoring and diet as well!
Web-DVM guest blogger Dr. Karen Louis is a practicing small animal veterinarian. See more of her articles at her blog at VetChick.com
As I was at the North American Veterinary Conference getting trained in acupuncture a few weeks ago and seeing first hand its benefits and practical applications, I really began to take a look at our western culture and how generally resistant it is to it and many other alternative treatment modalities. The first question I pondered was, why not explore and offer these treatment modalities as part of an integrative medical approach to patient wellness? In the process of mulling this around in my mind, in the past two weeks, two experiences/realizations made it abundantly clear exactly why our culture has heretofore been overwhelmingly dismissive of alternative medicine.
Before going further, it is first important to compare traditional western medicine with alternative medicine to provide a clear contrast of these different sides of medicine. Western medicine is predicated upon the notion of identifying the disease and treating it directly: a pill here, a surgical procedure there, and the patient gets better…a lot of the time. Alternative medicine is more geared toward boosting the body’s intrinsic ability to heal itself with modalities that include traditional Chinese medical alternatives such as herbal medicine and acupuncture, nutritional and nutraceutical therapy; as well as more high tech alternative options, such as low level laser tissue rehabilitation or electro-acupuncture.
The pros of the western approach is diagnostic capability (x-rays, blood work, ultrasound, blood pressure, etc.), often more immediate results, and the ability to save life through through the application of fluid therapy, pharmacological agents, and hemorrhage control. The main con of this approach is that application of these treatment modalities are frequently fraught with side effects. In the case of chronic disease, long term drug therapy can range from causing side effects that range from mild to severe or even life threatening. Invasive surgery can carry great risks are post-operative adverse effects that may last a lifetime.
The main pro of alternative medicine, is the management of disease without adverse side effects and often the ability to avoid invasive surgery and potentially harmful drug therapy. The main con is the lack of diagnostic capability to provided a concrete diagnosis, and often it lacks real strategies for saving life in times of crisis (acute trauma, hemorrhage, shock, etc.).
So which is better? Which one should we choose for ourselves and for our pets? The answer it each of these questions is, BOTH. The truth is that each branch of medicine has important practical application in treating disease and in the maintenance of wellness. This combination holistic approach is called integrative medicine, meaning that we address the disease, utilizing diagnostics and managing pain, inflammation and life threatening circumstances, but then for the long term look to support the “whole” patient with optimal nutritional considerations and any combination of supplements, herbal therapy, acupuncture, and low level laser therapy. That is what is best for the patient, and that is how everyone should be practicing medicine.
So why is this so often not the case? Why do doctors, instead of practicing integrative medicine, opt instead to draw lines in the sand and refuse to acknowledge that both forms of medicine have their place in maintaining the wellness of a patient? Well, ego probably plays a significant role in this circumstance, but I wish it were that simple.
The truth is, that there are two problems at work here. The first is that we live in a fast paced, results based society that often demands immediate results and wish for a simple injection or pill to make the patient better so that he.she may get on with his/her life. As an example, I have a friend who suffers from Crohn’s Disease, an often debilitating inflammatory disease of the gastrointestinal system. During times when he has taken the initiative to eat a well balanced diet with a lot of unprocessed fruits and vegetables, as well as probiotics (good GI bacteria) to promote good digestion, he has felt better and done better. But…he is a very busy man and is tired when he gets home from work, so rather take the time to prepare healthy meals for each day or even cook at home, he often survives on fast food and vending machine foods for sustenance, and to tolerate it, has to load up on antacid and GI anti-inflammatory pills for days at a time.
The other barrier for consideration of alternative therapy is from my view, the biggest obstacle: insurance companies. In veterinary medicine, we do not have to deal with health insurance companies nearly on the same level as on the human side, but a lot of innovation in veterinary medicine has its roots in human medicine. Pet owners’ expectations in the treatment of their pets also has its roots in their own experience with health care…they are less likely to be open to alternative medical therapy if none are ever offered for their own care. The bottom line is that human health insurance companies will not cover alternative medical therapy, so even in the cases of western trained doctors that see that value in it (there are many more than people realize), they will not offer it, as they are not willing to offer any forms of therapy that their patient’s insurance company will not pay for. I had a conversation with a human medical doctor just last week who is CEO of a company that runs five physical therapy locations in the county I live. When I mentioned to him that I offer low level laser therapy to my patients and asked if he offers it to his, he told me flat out no. He intimated that he is thrilled to see it gaining such momentum in veterinary medicine because the data is there that proves that it works, but he cannot offer it because none of his patients’ insurance plans will cover it, end of story
In my next post/episode, I will discuss practical applications of integrative medicine that I am using in my practice.
Dr. Roger Welton is the President of Maybeck Animal Hospital in West Melbourne, FL and founder/CEO of Web-DVM.net.
